Insights from Town Center Orthopaedics
Welcome to the Town Center Orthopaedics blog, your resource for expert guidance on musculoskeletal health, injury prevention, treatment options, and recovery. Our physicians and specialists share evidence-based insights to help you stay informed, make confident decisions, and stay active at every stage of life.
Whether you’re managing a new injury, considering treatment, or looking for ways to optimize your performance, our goal is to empower you with knowledge that supports your journey to Move Better. Feel Better. Be Better.
-

Bunions in Athletes: How Running, Dance, and Court Sports Affect Your Feet
Bunions in Athletes: How Running, Dance, and Court Sports Affect Your Feet
A powerful sprint down the track, a graceful leap across the stage, or a quick pivot on the basketball court all demand precision from your feet.
-
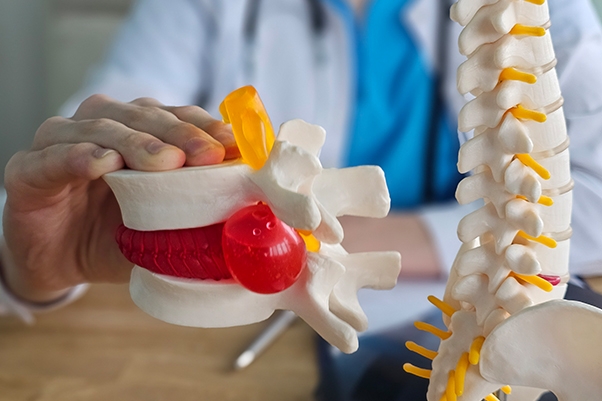
When Back Pain Comes From a Disc: Herniated Disc vs. Bulging Disc Explained
When Back Pain Comes From a Disc: Herniated Disc vs. Bulging Disc Explained
The human spine is a masterpiece of engineering, but even the strongest structures have vulnerable points.
-

Why Your Hands Go Numb at Night: Understanding Carpal Tunnel Syndrome
Why Your Hands Go Numb at Night: Understanding Carpal Tunnel Syndrome
Waking up with numb, tingling fingers is often dismissed as sleeping wrong, but it can signal a deeper issue.
-

Back to Work Faster: How Orthopedic Specialists Help Employees Recover Safely and Efficiently
Back to Work Faster: How Orthopedic Specialists Help Employees Recover Safely and Efficiently
When a workplace injury occurs, the clock starts ticking on both your physical recovery and your professional life. Navigating the complexities of a workers' compensation claim while managing a serious hip or knee injury can feel like a full-time job in itself.
-

From Elbow Tendonitis to Rotator Cuff Strains: When PRP Helps Chronic Tendon Injuries Heal
From Elbow Tendonitis to Rotator Cuff Strains: When PRP Helps Chronic Tendon Injuries Heal
Tendon injuries keep many athletes stuck in a frustrating loop-short-term relief followed by the same stubborn pain. A sharp pull in your shoulder during a serve or a persistent ache in your elbow between matches can quickly disrupt your tennis match, golf game, overall performance, and daily routine.
-

Shoulder Injuries in Skiers: Why Falls Lead to Dislocations and Labral Tears
Shoulder Injuries in Skiers: Why Falls Lead to Dislocations and Labral Tears
The exhilaration of carving down a pristine slope can quickly turn to agony with a single misstep or unexpected fall.
-
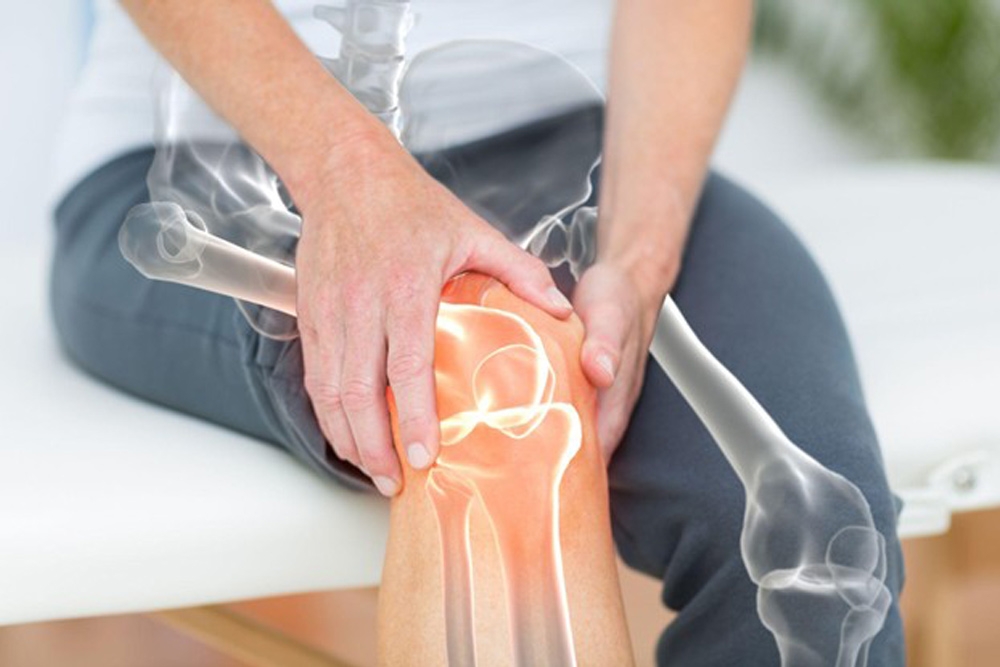
Precision Matters: The Benefits of Robotic Joint Replacement
Precision Matters: The Benefits of Robotic Joint Replacement
Hip and knee replacement surgery has come a long way from the days of one-size-fits-all solutions.
-

Wrist Sprains and Ligament Injuries in Stick Sports: Hockey, Lacrosse, and Field Hockey
Wrist Sprains and Ligament Injuries in Stick Sports: Hockey, Lacrosse, and Field Hockey
Being fast-paced, high-impact, and precision-driven, stick sports such as hockey, lacrosse, and field hockey challenge athletes to move with power and control.
-

Shoulder Pain in Sports: When It’s More Than Just Soreness
Shoulder Pain in Sports: When It’s More Than Just Soreness
A little shoulder soreness after practice is expected, but when that ache lingers or limits your motion, it could mean more than overworked muscles.
-

Understanding Acute vs. Chronic Orthopedic Pain: What Patients Should Know
Understanding Acute vs. Chronic Orthopedic Pain: What Patients Should Know
Pain is your body’s way of signaling that something isn’t right. Sometimes, it’s a brief warning that fades with rest and recovery;
-

Carpal Tunnel vs. Wrist Tendonitis: What’s Causing Your Pain?
Carpal Tunnel vs. Wrist Tendonitis: What’s Causing Your Pain?
Wrist pain can be tricky, especially for athletes and weekend warriors who love pickleball, tennis, or...
-

Benefits of Outpatient Hip and Knee Replacement Surgery
Benefits of Outpatient Hip and Knee Replacement Surgery
As the crisp fall season sets in, many people want to move more comfortably—whether it’s enjoying walks...